
SDG 3.a.1 Age-Standardized Prevalence of Current Tobacco Use Among Persons Aged 15 Years and Older was published by the CSO, Irish Health Survey.
Just under one in six (15%) of Irish people aged 15 and over were daily smokers in 2015. This proportion varied across the country, with the highest rate of 21% in the Midland region and the lowest rate of 12% in the Border. A further 7% of Irish people age 15 and over smoked occasionally in 2015. Overall, 22% of Irish people smoke daily or occasionally. See Table 6.1 and Map 6.1.
The prevalence of smoking fell from 23% to 17% between 2015 and 2019 among all people aged 15 and over.
Men are more likely to smoke than women. In 2015, 19% of men smoked compared with 16% of women.
Those aged between 25 and 34 years are the group with the highest proportion of smokers in Ireland. Just over one in four (26%) of those aged 25-34 years were smokers in 2019.
People living in deprived areas are more likely to smoke. The prevalence of smoking in deprived areas was 24% in 2019, ten percentage points higher than the rate of 14% in affluent areas. See Table 6.2 and Figure 6.1.
| X-axis label | 2015 | 2016 | 2017 | 2018 | 2019 |
|---|---|---|---|---|---|
| Total Population | 23 | 23 | 22 | 20 | 17 |
| Male | 24 | 26 | 25 | 22 | 19 |
| Female | 21 | 20 | 20 | 17 | 16 |
| Population in Affluent Areas | 16 | 16 | 16 | 16 | 14 |
| Population in Deprived Areas | 35 | 35 | 32 | 26 | 24 |
| Use of E-Cigarettes | 3 | 3 | 4 | 4 | 5 |
SDG 3.b.1 Proportion of the Target Population Covered by all Vaccines Included in Their National Programme was published by the Health Protection Surveillance Centre (HPSC).
Some of the main vaccines reported on by the HPSC are:
Diphtheria (D3) Vaccine
D3 is a vaccine against Corynebacterium diphtheriae, the bacterium that causes diphtheria. Diphtheria is an acute bacterial disease usually affecting the tonsils, pharynx, larynx and occasionally the skin. Diphtheria is a vaccine preventable disease. Its use has resulted in a more than 90% decrease in number of cases globally between 1980 and 2000. The first dose is recommended at six weeks of age with two additional doses four weeks apart, after which it is about 95% effective during childhood. Three further doses are recommended during childhood. It is unclear if further doses later in life are needed.
Pertussis (P3) Vaccine
P3 is a vaccine that protects against whooping cough (pertussis). There are two main types: whole-cell vaccines and acellular vaccines. The whole-cell vaccine is about 78% effective while the acellular vaccine is 71–85% effective. The effectiveness of the vaccines appears to decrease by between 2 and 10% per year after vaccination with a more rapid decrease with the acellular vaccines. Vaccinating the mother during pregnancy may protect the baby. The vaccine is estimated to have saved over 500,000 lives in 2002.
Haemophilus Influenzae Type B (Hib3) Vaccine
Hib3 is a vaccine used to prevent Haemophilus influenzae type b (Hib) infection. Hib is a bacterium that can cause serious infection in humans, particularly in children, but also in individuals with weakened immune systems. In countries that include it as a routine vaccine, rates of severe Hib infections have decreased more than 90%. It has therefore resulted in a decrease in the rate of meningitis, pneumonia, and epiglottitis.
Polio 3 Vaccine
Polio vaccines are vaccines used to prevent poliomyelitis (polio). Two types are used: an inactivated poliovirus given by injection (IPV) and a weakened poliovirus given by mouth (OPV). The World Health Organization (WHO) recommends all children be fully vaccinated against polio. The two vaccines have eliminated polio from most of the world and reduced the number of cases reported each year from an estimated 350,000 in 1988 to 33 in 2018.
Hepatitis B (HepB) Vaccine
HepB is a vaccine that prevents Hepatitis B. The first dose is recommended within 24 hours of birth with either two or three more doses given after that. This includes those with poor immune function such as from HIV/AIDS and those born premature. It is also recommended that health-care workers be vaccinated. In healthy people routine immunisation results in more than 95% of people being protected.
Pneumococcal Conjugate Vaccine (PCV)
PCV is a pneumococcal vaccine and a conjugate vaccine used to protect infants, young children and adults against disease caused by the bacterium streptococcus pneumoniae (pneumococcus). The World Health Organization (WHO) recommends the use of the conjugate vaccine in routine immunisations given to children.
Meningococcal (MenC) Vaccine
MenC vaccine refers to any of the vaccines used to prevent infection by Neisseria Meningitidis. Different versions are effective against some or all of the following types of meningococcus: A, B, C, W-135, and Y. The vaccines are between 85 and 100% effective for at least two years. They result in a decrease in meningitis and sepsis among populations where they are widely used. They are given either by injection into a muscle or just under the skin.
Pneumococcal Conjugate Vaccine (PCV)
PCV is a pneumococcal vaccine and a conjugate vaccine used to protect infants, young children and adults against disease caused by the bacterium streptococcus pneumoniae (pneumococcus). The World Health Organization (WHO) recommends the use of the conjugate vaccine in routine immunisations given to children.
Rota Vaccine
Rotavirus vaccine is a vaccine used to protect against rotavirus infections, which are the leading cause of severe diarrhea among young children. The vaccines prevent 15–34% of severe diarrhea in the developing world and 37–96% of severe diarrhea in the developed world. The vaccines decrease the risk of death among young children due to diarrhea. Immunizing babies decreases rates of disease among older people and those who have not been immunized.
MMR Vaccine
The MMR vaccine is a vaccine against measles, mumps and rubella (German measles). The first dose is generally given to children around 9 to 15 months of age, with a second dose at 15 months to 6 years of age, with at least 4 weeks between the doses. After two doses, 97% of people are protected against measles, 88% against mumps, and at least 97% against rubella. The vaccine is also recommended in those who do not have evidence of immunity, those with well-controlled HIV/AIDS, and within 72 hours of exposure to measles among those who are incompletely immunized. It is given by injection.
Table 6.3 and Figure 6.2 shows the National Annual Immunisation % Uptake Statistics at 24 Months, 2010 - 2018.
| X-axis label | 2018 |
|---|---|
| D3T3 | 94.5 |
| P3 | 94.5 |
| Hib3 | 94.5 |
| Polio3 | 94.5 |
| HepB3 | 94.4 |
| Hib4 | 85 |
| Hibb | 89.7 |
| MenB3 | 90.3 |
| MenB Complete | 92.2 |
| MenC2 | 86.7 |
| MenCb | 87.9 |
| PCV3 | 89.9 |
| PCVb | 91.5 |
| Rota2 | 90.3 |
| MMR1 | 92.3 |
The uptake of the influenza vaccine in all hospitals rose from 18.1% in 2011-2012 to 52.3% by 2018-2019. Over this same time period, the uptake in private hospitals increased from 22.0% to 41.7%. See Table 6.4.
SDG 3.b.2 Total Net Official Development Assistance to Medical Research and Basic Health Sectors was published by the Department of Foreign Affairs and Trade (DFA) in their Irish Aid Annual Report 2018.
Irish Aid (a division of DFA) is the Irish Government’s official aid programme, working on behalf of Irish people to address poverty and hunger in some of the world’s poorest countries. The aid programme is an integral part of Ireland’s foreign policy.
The Official Development Assistance (ODA) spent on health (including HIV/AIDS) was €41.7 million (5% of Total ODA) in 2018. See Table 6.5 and Map 6.2.

SDG 3.b.3 Proportion of Health Facilities that have a Core Set of Relevant Essential Medicines Available and Affordable on a Sustainable Basis.
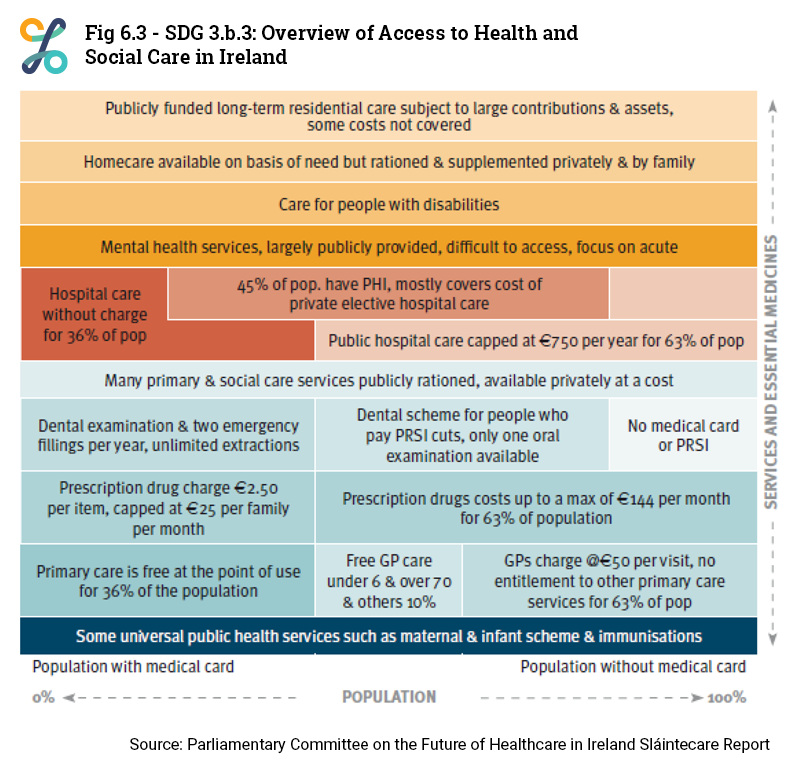
Ireland's Health Service Executive (HSE.ie) provides public health and social care services to everyone living in Ireland. In this Section a summary of current access to some health and social care services in Ireland are extracted from the parliamentary Committee on the Future of Healthcare in Ireland Sláintecare Report.
The Committee on the Future of Healthcare in Ireland outlined the long-term policy direction for Ireland’s healthcare system in the Sláintecare Report:
The Committee on the Future of Healthcare has specific Terms of Reference relevant to entitlement and access. The Terms of Reference state that there is a: …need to establish a universal single tier service where patients are treated on the basis of health need rather than on ability to pay.
In Ireland, there are virtually no universal entitlements to healthcare, only ‘eligibility’ for some services as specified in the 1970 Health Act. The 1970 Health Act divides all residents into two categories:
Category 1 – people with full eligibility (with medical cards) (36%)
Category 2 – people with limited eligibility (without medical cards) (64%)
Category 1 - People with Medical Cards
Approximately 32% of the population in Ireland in 2019 had medical cards (See SDG 3.8.1). Medical Cards allow people to get a wide range of health services and medicines free of charge.
Category 2 - People without Medical Cards
Those without medical cards (category 2) either access public hospital care free of charge (public outpatient appointment) or subject to a statutory charge (inpatient hospital care at €80 per day, capped at €800 per year). Non-medical card holders who present to the Emergency Department without a GP referral are charged €100 and they have to pay the full cost of visiting a GP (€52 on average per GP visit). Under the Drugs Payment Scheme (DPS), a person (or family) without a medical card pays up to €144 per month for prescription medication.
The Maternity and Infant Care Scheme
The Maternity and Infant Care Scheme was introduced in sections 62 and 63 of the 1970 Health Act making maternity care and infant care for the first six weeks of life free for all mothers and babies. This scheme is one of the only truly universal aspects of the current system. The HSE recently approved the National Healthy Childhood Programme which seeks to standardise supports to parents throughout childhood based on best international evidence.
Access to Primary and Social Care Services
In the 1970 Health Act (which still determines eligibility), there is an absence of clarity on access to care which is not GP or hospital provided. This means that for the whole population, there is a huge variety in access to primary and social care services depending on geographic location and existing supply in that area. Generally access to aids and appliances, public allied health professionals and Public Health Nurses (PHNs) are not available to those without medical cards, as noted by the Irish Heart Foundation.
GP Visit Cards (GPVC)
In 2005, a GP visit card (GPVC) was introduced which enables access to GP care without charge for those whose income is below a certain amount, but above the medical card threshold. In 2015, GP visit cards were introduced to all under six year olds and over 70 year olds. These allow GP visits without charge but critically do not provide access to essential medication, aids and appliances or the whole range of public primary and social care services to which a medical card facilitates access. Approximately 10% of the population had GPVCs in 2018 (See SDG 3.8.1).
Further information on health facilities in 2019 is published by the Department of Health.
SDG 3.c.1 Health Worker Density and Distribution was published by the Department of Health in Health in Ireland - Key Trends 2019.
The number of people employed in the public health service rose from 110,259 to 119,127 between 2016 and 2019, an increase of 8%. There were 24.2 public health service personnel per 1,000 population in 2019. The largest category of people employed in the public health service in 2019 was nursing at 31.8%, followed by other patient and client care at 21.5% and management/administration at 15.8%.
See Table 6.6 and Figure 6.4.
| SDG 3.c.1 Health worker density and distribution | |
| Medical/Dental | 9.01307008486741 |
| General Support | 7.96293031806392 |
| Other Patient & Client Care | 21.5433948643045 |
| Management/ Administration | 15.7890318735467 |
| Nursing | 31.766937805871 |
| Health & Social Care | 13.9246350533464 |
SDG 3.d.1 International Health Regulations (IHR) capacity and health emergency preparedness, is to 'Strengthen the capacity of all countries, in particular developing countries, for early warning, risk reduction and management of national and global health risks'. These data are classified as Tier 2 in the Tier Classification for Global SDG Indicators (See Background Notes ), as they are not regularly produced by countries. Metadata is provided here.
SDG 3.d.1 shows the percentage of attributes of 13 core capacities that have been attained at a specific point in time. The 13 core capacities are: (1) National legislation, policy and financing; (2) Coordination and National Focal Point communications; (3) Surveillance; (4) Response; (5) Preparedness; (6) Risk communication; (7) Human resources; (8) Laboratory; (9) Points of entry; (10) Zoonotic events; (11) Food safety; (12) Chemical events and (13) Radio nuclear emergencies.
In 2018, Ireland's IHR capacity was 100% (fully meets the essential public health capacity that countries are required to have) for 3 core capacities: Food Safety, Laboratory and Risk Communication. Legislation and Financing was 40% prepared for an emergency, which was the lowest score in 2018. See Table 6.7 and Figure 6.5.
| IHR Capacity | 2018 |
|---|---|
| Legislation and Financing | 40 |
| IHR Coordination and National IHR Focal Point Functions | 70 |
| Zoonotic Events and the Human�Animal Interface | 60 |
| Food Safety | 100 |
| Laboratory | 100 |
| Surveillance | 80 |
| Human Resources | 60 |
| National Health Emergency Framework | 80 |
| Health Service Provision | 67 |
| Risk Communication | 100 |
| Points of Entry | 0 |
| Chemical Events | 60 |
| Radiation Emergencies | 60 |
Go to next chapter: Background Notes
Learn about our data and confidentiality safeguards, and the steps we take to produce statistics that can be trusted by all.